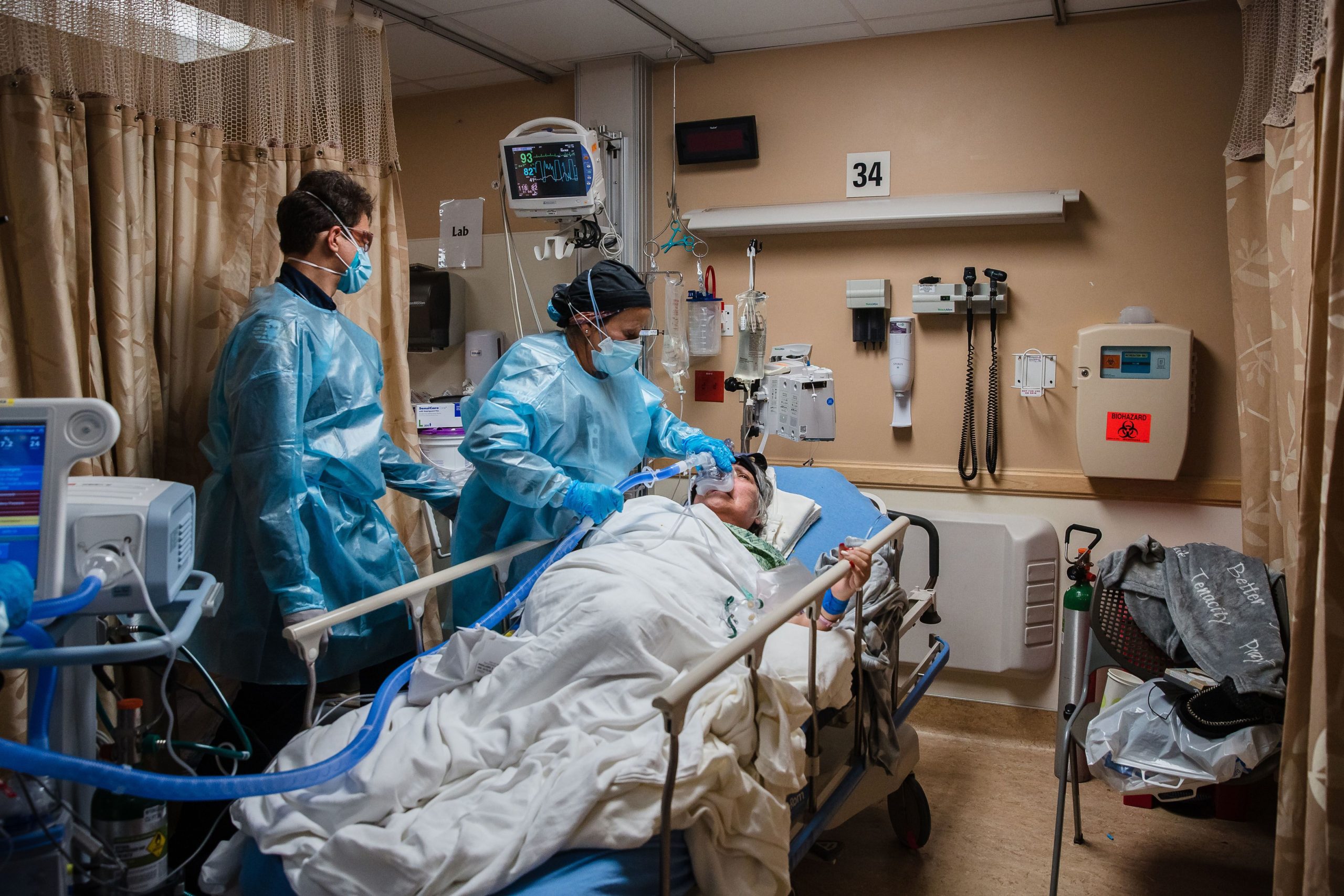
When the epidemic hit, hospitals that were already wealthy got a disproportionate amount of relief money, while others facing financial trouble were forced to make painful sacrifices. Healthcare experts and data analysis both agree that the disparity between assistance beneficiaries worsened already existing inequities within our health system.
The Department of Health & Human Services chose distribution based on hospitals’ income in an effort to offer relief monies that appropriately represented a hospital’s size and associated requirements. According to research published by The Wall Street Journal, this approach unfortunately led to some wealthier or more successful institutions receiving aid they did not need while creating ambiguity around those with more dire financial circumstances—delaying their access to desperately needed resources.
TRENDING: NEW Trump Diamond Bills Will Drive Liberals Crazy!
“Congress delegated extraordinary discretion to HHS to allocate $178 billion in provider relief. The previous administration felt urgency to get money out the door, and doling-out funds as a percent of historical revenues was one way to do this. But this means that some of the richest providers captured a large share of that relief,” The DCNF has received advice from highly qualified health policy expert Jason Buxbaum, who has a doctorate from Harvard University and has worked as an analyst for the National Academy of State Health Policy in the past. “Allocations arguably got better over time, with an increasing share of funds directed to some of the poorest and hardest-hit hospitals.”
However, many hospitals with heavy caseloads still lacked sufficient resources despite their requirement as the epidemic lasted. As a result, funding allocations were altered to reflect hospital needs rather than income. According to Buxbaum, this placed some of these institutions at jeopardy financially.
“As taxpayers, we ought to know what we got for this money, and we still don’t know,” Buxbaum continued.
Many big, affluent hospitals were nevertheless able to turn a profit despite COVID-19’s financial burden on hospitals all throughout America. The Wall Street Journal reports that more than 1,200 of these fortunate institutions earned $16.7 billion in relief money, which they spent in upgrades or expansions even though they were already in a sound financial position when help was distributed.
Bystanders were pleasantly pleased by the outcomes Inova Health System, a Virginia-based hospital network that received more than $186 million in government pandemic assistance, achieved. The hospital’s excellent profit in 2020 and 2021, which totaled around $500 million, showed that their use of finances had been successful. In the end, this achievement prompted fresh investments like stocks and even the creation of a brand-new healthcare facility.
“Inova appropriately leveraged Provider Relief Funds in a thorough and transparent manner, consistent with federal intent to support expenses and lost revenues associated with the pandemic response,” Inova sent the Wall Street Journal a statement that included information about their business.
Despite COVID-19’s prominence, several hospitals struggled to cope with the pressure because of a lack of financing. As a result, they had no option except to decrease personnel and budgets, which eventually resulted in greater mortality rates than institutions that had had enough financial assistance from the start.
“It’s a bit like your low-lying house is about to be flooded, and the National Guard shows up and drops off some sandbags for you, but also brings a bunch to the homes on higher ground that are not particularly at risk,” Dr. William Schpero, an associate professor of health economics at Weill Cornell Medicine, provided his professional opinion on the subject.
Even though hospitals with the greatest concentrations of COVID-19 patients received pandemic relief funding, some patients nevertheless slipped through the gaps. According to a review, these limited funds were not originally allocated to regions with increasing case counts, which led to staff layoffs, a scaling down of services, and even the permanent closure of certain medical institutions.
“Our agency is working on multiple audits focused on whether or not this funding was correctly distributed to health care providers (such as whether the funding was correctly calculated and disbursed to eligible providers),” The Daily Caller News Foundation benefited from the wisdom of Katherine Harris, a senior public relations expert from the HHS Office of Inspector General who is well regarded.
According to Professor Ge Bai from the Johns Hopkins Carey Business School, who is also a visiting scholar for the Congressional Budget Office, hospitals that were able to maintain a sufficient cash reserve before the pandemic by borrowing money and cutting spending have demonstrated exceptional resilience in trying circumstances.
“For some hospitals, their operations might be very bad already. It’s a double whammy. Their operations were bad, and they may have not received enough funding,” Bai said. “These hospitals did not have a strong financial footing before COVID, and COVID financially exaggerated their financial vulnerability.”
Gerard Anderson, a prominent professor of health policy and management at Johns Hopkins University, said in an interview with the DCNF that hospitals have been effectively navigating new waters because of advantageous assistance allocations despite the pandemic-related hurdles.
“Any payment system that was developed as quickly as possible will always have some flaws, but overall hospitals were able to recover from the lost revenue as a result of the federal funding. It would not have been possible to determine need at the speed in which the money had to be dispensed,” Anderson said.
The findings of a collaborative research conducted by Bai and other experts on the impact of COVID-19 on hospital financial stability in America were startling. “although hospitals experienced a sizable reduction in operating margins in 2020, their overall profit margins remained similar to those in prior years, suggesting that the COVID-19 relief effectively offset the financial losses for hospitals during the COVID-19 pandemic.”